15,200 Hospitals Stopped Cashless Treatment: If you’ve been following healthcare news, you probably caught the headline: 15,200 hospitals across India have stopped offering cashless treatment for Bajaj Allianz policyholders starting September 1, 2025. That’s right—fifteen thousand hospitals. This is one of the largest stand-offs in India’s healthcare insurance sector, and it impacts millions of families who rely on Bajaj Allianz for medical coverage. So, why did hospitals take such a drastic step? The dispute boils down to money, contracts, and systemic delays. But the real story is layered—it affects not just policyholders, but also doctors, hospital staff, and even India’s larger healthcare ecosystem. Let’s break this down in simple terms, while also exploring the professional side of the issue.
15,200 Hospitals Stopped Cashless Treatment
The suspension of cashless treatment at 15,200 hospitals for Bajaj Allianz policyholders is more than a contract dispute. It’s a spotlight on the fragile balance between hospitals, insurers, regulators, and patients. Hospitals demand fair compensation, insurers want affordability, and patients just want stress-free healthcare access. For policyholders, the best approach right now is to stay informed, keep emergency funds ready, and prepare for reimbursements. Because when it comes to healthcare, financial preparedness is as important as medical preparedness.

| Point | Details |
|---|---|
| Who is affected? | 15,200 hospitals across India, including Max Healthcare, Medanta, and PSRI. |
| Policyholders | Bajaj Allianz health insurance customers across India. |
| Main Reasons | Outdated reimbursement rates, inflation pressures, delayed payments, arbitrary deductions. |
| Start Date | September 1, 2025. |
| Impact | Patients must now pay upfront at these hospitals and later file for reimbursement. |
| Other Insurers at Risk | AHPI has warned Care Health Insurance with a similar suspension. |
| Regulatory Role | IRDAI is monitoring and may step in to mediate. |
| Official Reference | Bajaj Allianz Website |
What Does “Cashless Treatment” Mean?
In health insurance, cashless treatment allows patients to get hospitalized without paying upfront. The hospital and insurance company settle the bill directly. For patients, this means less stress, especially during emergencies.
But when cashless arrangements collapse, patients must pay the hospital themselves first and later claim reimbursement from the insurer. For many families, this is a financial nightmare.
Why 15,200 Hospitals Stopped Cashless Treatment?
Hospitals, represented by the Association of Healthcare Providers–India (AHPI), listed multiple reasons:
Outdated Reimbursement Rates
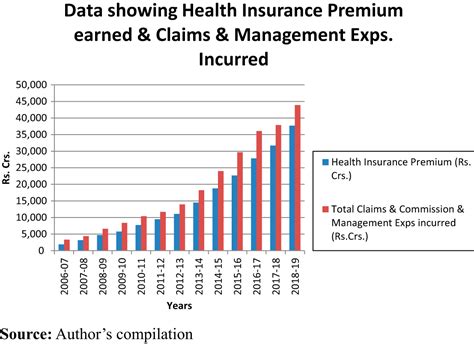
Medical costs in India rise about 7–8% every year. From doctors’ salaries to imported stents, everything costs more. Yet hospitals claim Bajaj Allianz continues to pay at old package rates, making treatments financially unviable.
For example: an angioplasty costing ₹2.5 lakh today may still be reimbursed at ₹1.5 lakh. Hospitals can’t make up the difference without cutting corners.
Arbitrary Deductions
Hospitals allege that insurers make unexplained cuts to claims. Even when bills are raised per contract, Bajaj Allianz often reimburses less. This erodes trust and leaves hospitals shouldering losses.
Payment and Approval Delays
Hospitals complain about long settlement times. Claims drag on, and patients often wait for pre-authorizations and discharge approvals. This not only impacts finances but also causes emotional stress for patients and families.
Pressure for Further Tariff Reductions
Even after contracts expired, Bajaj Allianz allegedly demanded further cuts. Hospitals argue that while patients deserve affordable care, unrealistic pricing threatens their ability to maintain quality standards.
A Real-World Example: Rajesh’s Story
Rajesh, a 45-year-old IT professional in Delhi, has a Bajaj Allianz family floater policy. When his father needed urgent bypass surgery at Medanta, Rajesh assumed his cashless policy would cover the cost.
But after September 1, 2025, Rajesh must arrange nearly ₹5 lakh upfront. He’ll eventually get reimbursed, but not before arranging funds. For middle-class families, that often means loans, credit cards, or borrowing from relatives. The stress of arranging money can overshadow the medical crisis itself.
The Scale of the Suspension
This isn’t just about small clinics—it includes 15,200 hospitals nationwide, with many top private hospitals on the list:
- Max Healthcare
- Medanta
- Pushpawati Singhania Research Institute (PSRI)
- Numerous regional and district-level private hospitals
For Bajaj Allianz policyholders, this is a massive network loss, affecting routine and emergency healthcare.
Historical Context: Not the First Showdown
Conflicts between insurers and hospitals aren’t new. In 2010, several top hospitals in Delhi and Mumbai briefly cut ties with insurers due to disputes over low package rates. Government intervention at the time restored services.
Internationally, the U.S. sees similar disputes, often leaving patients with “out-of-network” bills. In Europe, stricter regulations help prevent large-scale breakdowns, though disputes still occur behind closed doors.
Regulatory Role: Can IRDAI Step In?
The Insurance Regulatory and Development Authority of India (IRDAI) oversees health insurance in India. It has the power to:
- Mandate revised tariffs or fair pricing models.
- Ensure hospitals and insurers follow timely claim settlement standards.
- Protect consumer rights by monitoring disputes.
While IRDAI has not yet issued a directive, many experts expect the regulator to step in if negotiations fail.
Impact Beyond Patients: Doctors and Hospitals
It’s not just about bills. Delayed or reduced payments impact hospitals internally:
- Doctors face pressure to shorten treatment cycles.
- Nurses and paramedical staff may see resource cuts.
- Hospitals delay upgrading critical equipment due to financial strain.
The suspension of cashless facilities, therefore, is as much about quality of care as it is about money.
What Policyholders Should Do Right Now?
If you’re a Bajaj Allianz policyholder, here’s how you can prepare:
1. Check the Latest Network List
Use the Bajaj Allianz hospital network tool to confirm if your preferred hospital still offers cashless treatment.
2. Be Ready for Reimbursement
Always save discharge summaries, bills, and test reports. Scan them digitally to avoid losing paperwork. Insurers usually allow 30–60 days for filing reimbursement claims.
3. Maintain an Emergency Fund
Even ₹1–2 lakh in liquid savings can ease stress if you need to pay upfront. Consider short-term health loans as a backup.
4. Stay Updated on Negotiations
Hospitals may restore cashless facilities if agreements are revised. Keep tabs on Bajaj Allianz announcements and AHPI press releases.
Could Other Insurers Face the Same Fate?
Yes. AHPI has already warned Care Health Insurance that they face suspension if they don’t revise tariffs by August 31, 2025. If more insurers clash with hospitals, India could see a ripple effect, forcing systemic reforms in how tariffs and settlements are negotiated.
The Professional Angle: Why This Matters for the Healthcare Industry
For professionals in healthcare, finance, and insurance, this standoff highlights deeper issues:
- Sustainability of insurance pricing: Insurers want affordable premiums, but hospitals demand fair compensation.
- Patient trust: If patients lose faith in cashless systems, insurance uptake could slow down.
- Need for transparent contracts: Hospitals and insurers must move toward dynamic, inflation-linked pricing.
Industry experts argue that India’s healthcare sector needs standardized, transparent tariffs regulated by IRDAI, much like Medicare rates in the U.S.
Insurance Stocks Surge on GST Exemption Talk – Should Investors Buy In Now?
GST on Health and Term Insurance May Drop to Just 5%- What We Know So Far
Zero GST on Health & Life Insurance Proposed – Will Your Premiums Finally Drop?
The Road Ahead: Possible Outcomes
There are three possible scenarios in the coming months:
- Successful Negotiations: Bajaj Allianz revises tariffs, hospitals restore cashless services, and patients breathe easier.
- Prolonged Standoff: Hospitals continue suspending cashless services, forcing patients into reimbursement mode.
- Regulatory Intervention: IRDAI enforces standardized tariffs and timelines, setting a precedent for future disputes.
Whichever path unfolds, the outcome will shape how India balances affordable insurance with sustainable healthcare delivery.










